May 2015
Authors: Morgan Cowan MD and Christopher J. VandenBussche MD PhD, Department of Pathology, The Johns Hopkins University School of Medicine, Baltimore, Maryland, USA.
Reviewer: Syed Z. Ali MD FRCPath FIAC, Department of Pathology, The Johns Hopkins University School of Medicine, Baltimore, Maryland, USA.
Case:
A 67 year old woman with a history of diastolic heart failure, pulmonary hypertension, diabetes mellitus type II, and prior resection of meningioma with subsequent neurogenic bladder presented to the emergency department with nausea, diarrhea, and abdominal pain. A CT scan revealed a 10 cm liver mass and multiple smaller masses with features suggestive of hemangioma. Six weeks later, the patient saw a surgeon in consultation for presumed hemangiomas, but was admitted for worsening heart failure and volume overload. Repeat scans showed interval enlargement of the masses and development of new masses, and on MRI the lesions exhibited T2 hyperintensity, T1 hypointensity, and enhancement characteristic of a hemangioma. Biopsy was recommended for a definitive diagnosis. An ultrasound-guided fine needle aspiration with core biopsy was performed.
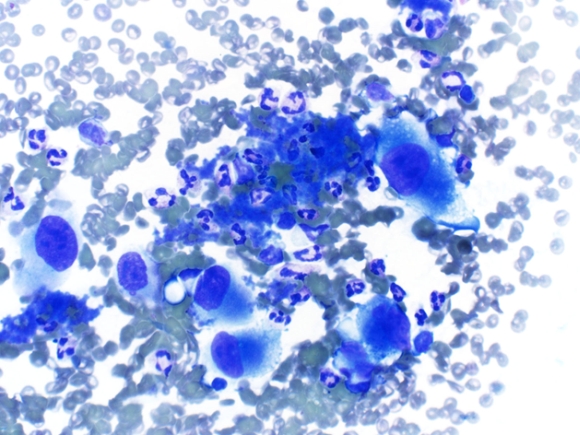 |
| Fig. 1 |
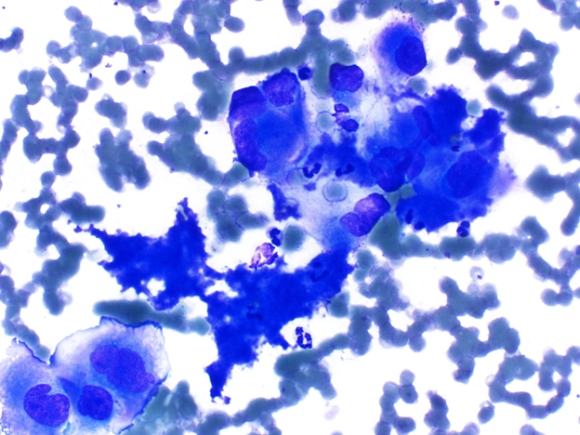 |
| Fig. 2 |
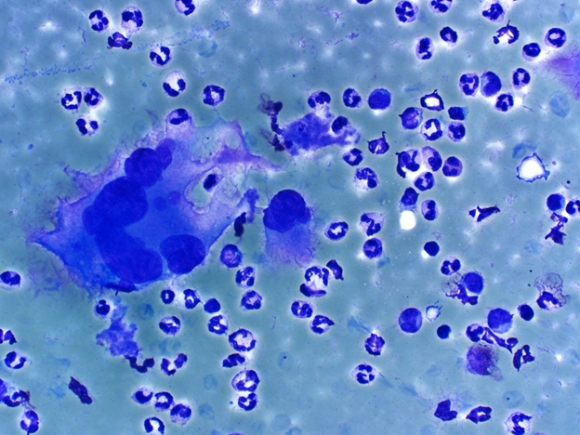 |
| Fig. 3 |
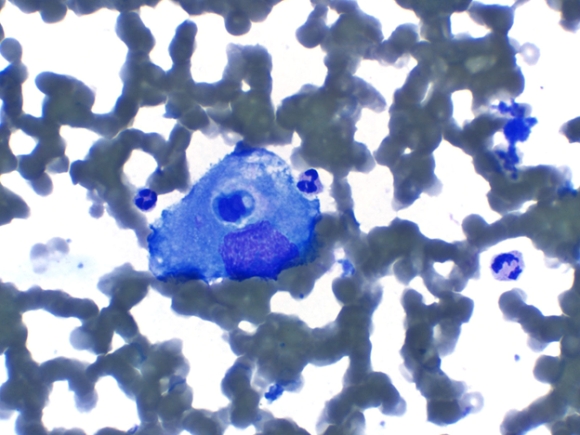 |
| Fig. 4 |
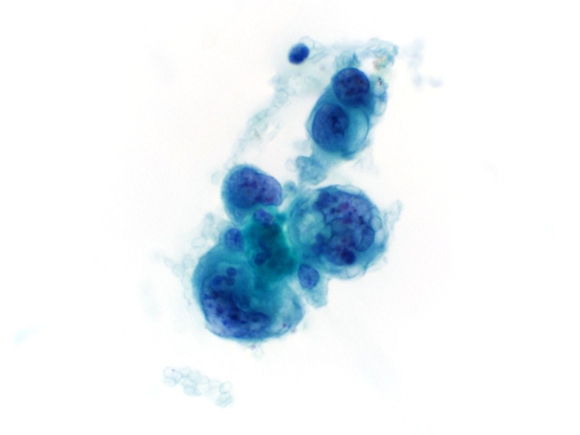 |
| Fig. 5 |
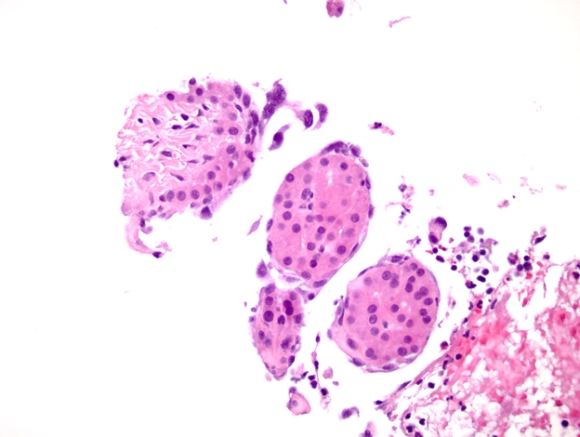 |
| Fig. 6 |
Question:
Based on the cytomorphology, which of the following is the best diagnosis?